Epidural Steroid Injections vs. Surgical Options for Spinal Conditions
Spinal conditions can cause excruciating pain and significantly impact one's quality of life. Whether it's a herniated disc, spinal stenosis, or other issues, individuals facing spinal problems often seek relief through medical interventions. Two common approaches to managing spinal conditions are Epidural Steroid Injections (ESIs) and surgical procedures.
Understanding Exploring Comparing Weighing Considerations Conclusion
Understanding ESIs
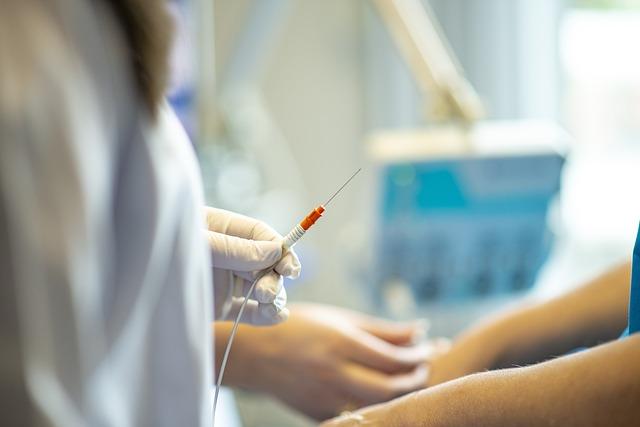
Epidural Steroid Injections (ESIs) are a non-surgical treatment option to relieve pain and inflammation associated with spinal conditions. These procedures entail injecting corticosteroids right into the epidural area that surrounds the spinal cord. Reducing inflammation, relieving pain, and enhancing general spinal function are the main objectives of ESIs. ESIs can provide patients with significant relief without requiring invasive surgery by focusing on the cause of pain and inflammation.
ESIs are typically performed as an outpatient procedure, and they can be administered in various ways, including cervical, thoracic, or lumbar epidural injections, depending on the location of the spinal condition. They are often recommended for herniated discs, spinal stenosis, sciatica, and radiculopathy.
Exploring Spinal Surgeries
Surgical interventions for spinal conditions encompass a broad spectrum of procedures, ranging from minimally invasive techniques to extensive spinal fusion surgeries. The choice of surgery depends on the specific diagnosis, the severity of the condition, and the patient's overall health. Some standard surgical options for spinal conditions include:
Discectomy:
This procedure involves removing a herniated or damaged disc, relieving pressure on spinal nerves, and reducing pain.
Spinal Fusion:
Spinal fusion stabilizes the spine by fusing two or more vertebrae using bone grafts, screws, or rods. It is often recommended for conditions like degenerative disc disease or spinal instability.
Laminectomy:
Laminectomy involves the removal of the lamina (the back part of a vertebra) to relieve pressure on the spinal cord or nerves. It is commonly used to treat spinal stenosis.
Artificial Disc Replacement:
In this procedure, a damaged disc is replaced with an artificial one, preserving motion in the spine. It's an alternative to spinal fusion for some patients.
Micro Discectomy:
A minimally invasive approach to remove herniated disc material, reducing damage to surrounding tissues and promoting quicker recovery.
Comparing Outcomes
When comparing the outcomes of Epidural Steroid Injections (ESIs) and surgical options for spinal conditions, several factors come into play:
Effectiveness:
ESIs can relieve pain significantly for many patients, especially those with acute or moderately severe symptoms. However, their effects may be temporary and require multiple injections. In contrast, surgical procedures often aim for more lasting relief, but the success rates can vary depending on the specific surgery and individual patient factors.
Recovery Time:
ESIs typically have minimal downtime, with most patients able to resume regular activities shortly after the procedure. Surgical recovery times vary widely, with minimally invasive techniques often allowing for faster recovery than extensive spinal fusions, which may require months of rehabilitation.
Long-Term Outcomes:
Surgical options may offer a more definitive solution to certain spinal conditions, potentially reducing the likelihood of future relapses. ESIs, while effective in the short term, may require ongoing injections to maintain pain relief.
Complications:
Both ESIs and surgeries come with inherent risks. ESIs may have minor side effects like temporary pain at the injection site, while surgeries can involve more significant risks such as infection, blood clots, or nerve damage.
Weighing Risks and Benefits
Weighing the risks and benefits is critical in making informed medical decisions, particularly when considering treatment options for spinal conditions such as Epidural Steroid Injections (ESIs) versus surgical interventions. This process involves a careful evaluation of both the potential advantages and drawbacks associated with each choice. Let's delve into this aspect in more detail:
ESIs Benefits:
Non-Surgical Approach:
One of the primary benefits of ESIs is that they offer a non-surgical solution for managing spinal conditions. This can especially appeal to individuals who wish to avoid the risks and extended recovery associated with surgery.
Minimally Invasive:
ESIs are minimally invasive procedures that typically involve a needle injection. They are less traumatic to the body compared to surgery, leading to less tissue damage and often a shorter recovery period.
Short Recovery Time:
Patients receiving ESIs typically experience a relatively short recovery time. They can usually return to their regular activities soon after the procedure.
Can Provide Relief for Some Patients:
ESIs can effectively reduce pain and inflammation in many cases, offering significant relief for patients with certain spinal conditions, especially when the source of pain is related to inflammation around nerves.
ESIs Risks:
Temporary Relief: One of the primary drawbacks of ESIs is that their pain relief may be temporary. While they can offer immediate relief, the effects may wear off over time, necessitating repeated injections for ongoing management.
May Require Repeated Injections:
ESIs may need to be administered regularly for some patients to maintain pain relief. This can be inconvenient and may not be a suitable long-term solution.
Limited Effectiveness for Certain Conditions:
ESIs may not be as effective for all spinal conditions. In cases where the source of pain is structural, such as severe disc degeneration or spinal instability, ESIs may not provide sufficient relief.
Surgical Benefits:
Potential for Long-Term Relief:
Surgical interventions often offer the potential for more lasting relief by addressing the root cause of the spinal condition. This can reduce the likelihood of recurrent symptoms and the need for ongoing treatment.
Address the Root Cause:
Surgery can directly address structural issues like herniated discs, spinal stenosis, or instability, providing a definitive solution to the problem.
Improved Spinal Stability:
Some surgical procedures, such as spinal fusion, can enhance spinal stability, which can be particularly beneficial for patients with conditions that result in spinal instability.
Surgical Risks:
Invasive Procedures:
Surgical interventions are inherently invasive and involve making incisions, which can lead to complications such as infection, bleeding, or scarring.
Longer Recovery Time:
Compared to ESIs, surgical procedures typically have a longer recovery period, which may involve weeks or even months of rehabilitation and restrictions on physical activity.
Potential for Complications:
Surgery carries inherent risks, including the possibility of nerve damage, infection, blood clots, and anaesthesia-related complications. The specific risks can vary depending on the type of surgery and individual patient factors.
Patient Considerations
Patient considerations are crucial when deciding between Epidural Steroid Injections (ESIs) and surgical options for spinal conditions. The choice between these two approaches should consider several factors unique to each patient's circumstances. Here are two key aspects to consider:
Severity of Condition:
The severity of the spinal condition is a pivotal factor in determining the most appropriate treatment. For patients with mild to moderate spinal issues, ESIs may be a viable option. Epidural steroid injections New Jersey can provide effective pain relief and reduce inflammation, making them particularly suitable for individuals with less severe conditions or those experiencing acute symptoms. On the other hand, for patients with severe spinal problems such as advanced disc degeneration, significant spinal instability, or debilitating pain, surgery may be the more appropriate choice. Surgical interventions can potentially address the root cause of these complex issues, offering a more comprehensive and long-lasting solution.
Patient Health:
A patient's overall health and medical history play a significant role in treatment decisions. Some individuals may have underlying health conditions that make surgery riskier due to potential complications or slower recovery. These conditions may include heart disease, diabetes, or a compromised immune system. ESIs might be a safer alternative in such cases because they are minimally invasive and typically associated with fewer post-procedural complications. Conversely, individuals in good overall health may be better candidates for surgery, as their bodies are better equipped to handle surgical interventions' physical demands and potential risks. Healthcare providers will carefully assess a patient's medical history and health status to make personalized recommendations.
Patient Preferences:
Patients' preferences and goals for treatment should also be considered. Some individuals may have a strong choice for non-surgical approaches and may be willing to accept the potential need for repeat injections if it means avoiding surgery. Others may prioritize a more definitive solution, even if it means undergoing a surgical procedure with a longer recovery time. Open and honest communication between patients and healthcare providers is essential to ensure that the chosen treatment aligns with the patient's preferences and values.
Medical Advice:
Consulting with a spine specialist or orthopaedic surgeon is critical in decision-making. These healthcare professionals can conduct a thorough evaluation, including imaging studies and diagnostic tests, to assess the spinal condition's nature and severity accurately. Based on this assessment, they can provide expert guidance on the most appropriate treatment options, considering the patient's unique circumstances. Patients should actively engage in discussions with their healthcare providers, asking questions and seeking clarification to make well-informed decisions about their spinal care.
Conclusion
In spinal conditions, Epidural Steroid Injections (ESIs) and surgical options have their places. ESIs offer a non-surgical alternative that can provide effective pain relief for many patients, especially those with less severe conditions. On the other hand, surgical interventions can address the root causes of spinal problems and offer more lasting relief.
Thank you Johny Kershaws for contributing this article.
Guest Articles Written for Caregiverology
From Epidural Steroid Injections vs. Surgical Options for Spinal Conditions to Home
Recent Articles
-
Common Truck Crash Injuries and Legal Remedies - Caregiverology
Jul 19, 25 10:49 AM
Known for its sun-drenched beaches, vibrant arts scene, and bustling maritime industry, Fort Lauderdale is a city that sees heavy traffic both on its roads and at its busy port. Unfortunately, with th… -
Why Expert Legal Help Matters After Serious Injury - Caregiverology
Jul 19, 25 10:35 AM
In Houston, over 67,600 car crashes occurred in 2023, resulting in 290 fatalities and 1,612 serious injuries. That’s roughly 185 accidents every day. -
How Life Care Planners Support Injury Recovery - Caregiverology
Jul 19, 25 10:18 AM
In Los Angeles, life care planners play a vital role in supporting injury recovery, especially for individuals facing catastrophic injuries such as traumatic brain injuries or spinal cord damage.




New! Comments
Have something to say about what you just read? Leave a comment in the box below.